Important basic principles in voice rehabilitation in prosthetic speechIn the beginning, voice therapy should focus on four general issues: airtight stoma occlusion, upright body position, abdominal breathing, and breath-voice coordination.
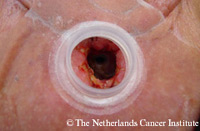
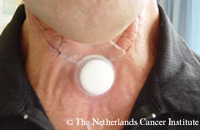
The acquisition of an airtight occlusion of the tracheostoma during phonation is important. In case the stoma is not yet well healed or is too large in relation to the patient’s finger size, airtight digital occlusion might pose a problem at this stage. The availability of special, valved-HME’s nowadays may eliminate this problem to a great extent (Ackerstaff, Hilgers, Balm, & Tan, 1998; Van As, Hilgers, Koopmans-van Beinum, & Ackerstaff, 1998). The pictures and video clip show an example of this (11 days) postoperative situation. These devices are often provided to patients shortly after surgery. As alternative method, a gauze covered small balloon could be used to achieve airtight occlusion of the stoma. As a reaction to non-airtight stoma occlusion, the patient may exert too much pressure on the stoma, hence, forcing the prosthesis against the posterior pharyngeal wall and obstructing airflow. Another unfavorable side effect of non-airtight stoma closure is the occurrence of disturbing stoma noise. In order to obtain a good occlusion with only a light pressure on the stoma, the patient is advised to bring the stoma, or the body weight towards the finger, instead of pressing the finger onto the stoma. An additional advantage of using a valved-HME is that the pressure placed on the stoma is more evenly distributed. An upright, relaxed body position is important for a good breath support. The back should be straight and the head bend forward just a little to avoid tension in the neck region around the stoma. Therefore, practicing while seated on a chair is preferred over sitting in bed early in therapy. A calm, abdominal breathing pattern, gentle abdominal inhalation before phonation and an easy, unforced expiration is necessary to obtain a good and relaxed voice. We advise observing the breathing pattern of the patient before starting breathing exercises, since some patients already use a good abdominal breathing pattern. In these patients, the therapist’s role is to make them aware of their abdominal breathing, whereas in those with a thoracic breathing pattern, breathing-exercises should be integrated in the speech therapy program. Good breath-voice coordination and timing of stoma occlusion are important factors, since stoma noise may occur when the patient closes the stoma too late at the beginning of a sentence, or releases finger pressure too early at the end of a sentence. When short sentences are formed easily and fluently, exercises are extended by trying longer phrases starting with any initial vowel or consonant. Speech becomes more fluent by using meaningful sentences, instead of just a list of words. |